[ Home ] [ Controlled Substances ] [ Opioids ]
METHADONE
|
Methadone, sold under the brand names Dolophine among others, is an synthetic opioid that is used as the hydrochloride to treat pain and as maintenance therapy or to help with detoxification in people with opioid dependence. Methadone hydrochloride is a mu-agonist; a synthetic opioid analgesic with multiple actions qualitatively similar to those of morphine. Some data also indicate that methadone acts as an antagonist at the NMDA-receptor. The contribution of NMDA receptor antagonism to methadone's efficacy is unknown. Most common adverse reactions are: lightheadedness, dizziness, sedation, nausea, vomiting, and sweating. Avoid use mixed agonist/antagonist and partial agonist opioid analgesics with DOLOPHINE because they may reduce analgesic effect of DOLOPHINE or precipitate withdrawal symptoms.
 Methadone:
Methadone:
https://drugs.ncats.io/drug/UC6VBE7V1Z
Methadone is a synthetic (man-made) narcotic. It is used legally to treat addiction to narcotics and to relieve severe pain, often in individuals who have cancer or terminal illnesses. Although methadone has been legally available in the United States since 1947, more recently it has emerged as a drug of abuse. This trend may be driven in part by the ready availability of the drug as it increasingly is used in the treatment of narcotic addiction and to relieve chronic pain.


https://www.justice.gov/archive/ndic/pubs6/6096/6096p.pdf
Why is this medication prescribed?
Methadone is used to relieve severe pain in people who are expected to need pain medication around the clock for a long time and who cannot be treated with other medications. It also is used to prevent withdrawal symptoms in patients who were addicted to opiate drugs and are enrolled in treatment programs in order to stop taking or continue not taking the drugs. Methadone is in a class of medications called opiate (narcotic) analgesics. Methadone works to treat pain by changing the way the brain and nervous system respond to pain. It works to treat people who were addicted to opiate drugs by producing similar effects and preventing withdrawal symptoms in people who have stopped using these drugs.

https://medlineplus.gov/druginfo/meds/a682134.html
What Does It Do?
Methadone changes the way your brain and nervous system respond to pain so that you feel relief. Its effects are slower than those of other strong painkillers like morphine. It blocks the high you get from drugs like codeine, heroin, hydrocodone, morphine, and oxycodone. Your doctor may prescribe methadone if you're in a lot of pain from an injury, surgery, or chronic illness. It can also help if you're in treatment for addiction to other opioids. It can give a similar feeling and prevent withdrawal symptoms. You may hear this called replacement therapy. Methadone replaces the opioids in your system with milder effects.
It's usually used as one part of your treatment plan. It isn't a cure for addiction.
https://www.webmd.com/mental-health/addiction/what-is-methadone
History:
The chemical structure of methadone was first produced in the 1930's as a team of German scientists was searching for a pain-killing drug (analgesic) that would not be as addictive as morphine. In 1937, two scientists (Max Bockmhl and Gustav Ehrhart) uncovered a synthetic substance that they called Hoechst 10820 or polamidon. Years later during World War II another team of German scientists expanded on earlier research and began synthesizing the substance as a result of short supplies of morphine and other analgesics. By the end of the war, the United States had obtained the rights to the drug from war requisitions and later coined the name methadone. Soon after in 1947 methadone was introduced into the United States to be used as a pain reliever for a variety of conditions, but eventually uncovered its usefulness in treating narcotic addictions. Until the 1960's, little scientific advancement was made with regard to methadone. But with a resurgence of heroin addiction, researchers began to search for a substance that could reduce or eliminate drug craving and withdrawal signs and symptoms. The idea behind this research was that methadone could be used to manage or maintain heroin addiction. In 1964, the effectiveness and usefulness of using methadone maintenance (i.e., using it as a substitute narcotic to prevent withdrawal) was realized. In the spring of 1971, methadone treatment for opiate dependence began to expand. That year the Federal Government developed regulations governing the use of methadone in the treatment of heroin addiction; final regulations were published in December 1972. Few advancements were made until 2001 when regulations over methadone were modified to allow physicians and other health care professionals to provide methadone more effectively and consistently.
Methadone's usefulness in treating heroin addiction:
Discovered in the 1960s. It is now routinely used on a daily, long-term (maintenance) basis as a substitute drug given to persons who were formerly or who would otherwise be addicted to heroin. It is given orally once a day. Methadone's usefulness as a heroin substitute stems from several important effects the drug has. First and foremost, when taken daily it prevents a former heroin addict from feeling withdrawal symptoms and it suppresses his drug hunger for heroin. Second, methadone itself causes no euphoric effects whatsoever, unlike heroin, so the person feels no disruptive psychological craving for it. Third, the human body does not develop a tolerance for methadone, unlike heroin, so methadone doses of the same (rather than increasing) size can be taken for long periods of time. Fourth, when used on a maintenance basis, methadone actually blocks the euphoric effects, or "high," produced by heroin, thus robbing this drug of its psychological attractiveness to the former addict. Finally, methadone's lack of euphoric effects and its 24-hour period of action enable persons maintained on it to lead relatively normal lives involving work, schooling, and normal family and social relations.

https://www.britannica.com/science/methadone
Detoxification:
Methadone detoxification involves the short-term administration of methadone hydrochloride to blunt the abstinence symptoms of patients who are dependent on opiates and then tapering the dose of methadone with the goal of achieving a drug-free state. The major disadvantage of detoxification in these patients is the high recidivism rate of heroin misuse after completing detoxification. The high recidivism rate may be attributed to a physiologic state and abstinence syndrome that persists long after long-term opiate use ceases. For detoxification, treatment doses are usually started at 10 to 20 mg and increased in 10-mg increments until the withdrawal symptoms are controlled. A dosage of 40 mg a day controls the withdrawal symptoms for most patients but does not eliminate heroin craving. Once the dose required is established to eliminate withdrawal symptoms, the patient is stabilized on this dose for 2 to 3 days. Then the dose is reduced daily or every other day. A 10% to 20% dose reduction is usually tolerated, but this must be tailored for each patient. If patients are experiencing abstinence symptoms or have a high risk of relapsing into heroin misuse, the practitioner should consider increasing the dose and slowing the tapering schedule. Individual tapering schedules may vary from weeks to months. Patients should be monitored for withdrawal symptoms after the discontinuation of methadone, bearing in mind that withdrawal symptoms may not be evident for 48 to 72 hours following their previous dose.

https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1070723/
Methadone Maintenance:
Methadone was first discovered in 1965 through the groundbreaking research of scientists at the Rockefeller Institute. Those early studies demonstrated methadone's remarkable ability to alleviate withdrawal and craving and improve the ability to function emotionally and socially. In the subsequent decades, the evidence supporting methadone's positive effects has grown. These include significant reductions in drug use, new HIV infection, crime, and death from overdose. The research is so strong that methadone, along with buprenorphine (Suboxone), has been added to the World Health Organization's list of essential medications. And yet despite this, only a minority of programs offer methadone treatment and the undeserved shame associated with this lifesaving medication persists.
Because there is a risk of diversion to the illicit market, program enrollees must come to specialized clinics for methadone for their daily dose. A single dose lasts 24 - 36 hours. Some methadone clinics also provide other medical and social services. There are few side effects. However, methadone can cause a potentially life threatening heart rhythm problem. It's rare and the risk can be minimized by periodically checking an electrocardiogram for a finding called prolonged QT interval.
Methadone can be continued indefinitely, or the dose can be gradually reduced in preparation for withdrawal. It has been estimated that about 25% of patients eventually become abstinent, 25% continue to take the drug, and 50% go on and off methadone repeatedly.

https://www.health.harvard.edu/mind-and-mood/treating-opiate-addiction-part-i-detoxification-and-maintenance
Treatment Regimen:
In maintenance treatment of opiate addicts, methadone is administered as a single constant daily dose after the induction period is over. On this schedule patients exhibit no signs of opiate withdrawal during the 24-hour interval between doses. If a daily dose is missed or omitted, however, a patient on methadone maintenance will exhibit signs and symptoms of opiate withdrawal, usually within 24 to 36 hours after the last dose of methadone. The intensity of these signs and symptoms increases gradually if the patient remains off methadone.
https://www.nap.edu/read/4899/chapter/4
How Methadone Clinics Work:
Initial Screening: Anyone can walk into an MMT clinic and request treatment. Initial screening exams and interviews determine the applicant's eligibility and the process includes an assessment of their readiness to accept treatment.
Admission Issues: A significant delay between the first contact, initial screening, and methadone treatment, especially failure to quickly address withdrawal, adversely affects the number of applicants who enter the program. It's difficult to deal with an opioid addict in withdrawal; his patience wears thin, and he wants treatment now. Recognizing the realities of crowding and limited resources, MMT clinics can provide an interim maintenance program without formal screening or actual admission to the site. By federal regulation, medication can be administered for up to 120 days with only minimal screening procedures. Violent or threatening patients can be turned down
Information, Collection, and Dissemination: During the first few visits, a substance abuse history is obtained, and treatment options are discussed. Consent to treat is elicited, and addicts must sign a bevy of documents that provide further information on the multifaceted MMT process. Patients must be 18 or have parental approval. Otherwise, the services are confidential even to family members. Confidential information is not given to any inquiry except the court.
Medical Assessment: The aim of medical assessment is to determine the safety of methadone use. The drug is often dispensed on the first visit because of withdrawal. It is generally required that someone be addicted for one year before admission.

https://journals.lww.com/em-news/fulltext/2009/04000/How_Methadone_Clinics_Work.16.aspx
Is methadone maintenance treatment effective for women?
Question 9: Answer: Yes. Since the earliest methadone maintenance treatment programs in the United States, women have been treated successfully with methadone through all phases of their lives, including pregnancy. There is consensus that the major outcomes of the effectiveness of methadone maintenance treatment, especially cessation of illicit drug use and lifestyle stabilization, apply to both men and women. However, gender-specific issues, which are often related to the social status of women, are important to treatment effectiveness for female injection drug users.

https://www.drugabuse.gov/sites/default/files/pdf/partb.pdf
Dangers of methadone:
Best known as a medication to help fight addiction, methadone represents only 2 percent of all opiate painkillers prescribed in the U.S. But it is involved in one out of every three accidental overdose deaths. As prescription drug overdose deaths soar nationwide, most states have failed to take a simple step that would make it harder for doctors to prescribe the deadliest of all narcotics. Unlike other narcotic pain medications, methadone depresses heart and lung activity long after its pain relief has stopped. Pain relief lasts four to eight hours, while potentially harmful respiratory depression can last up to 59 hours. In addition, experts say it is the most addictive of all opiates. The American Academy of Pain Medicine recommends that all insurers remove methadone from preferred drug lists, cautioning that it "has unique pharmacologic properties that call for caution and expertise in administering it." The CDC warns that methadone should not be considered a drug of first choice for chronic pain and it should never be used for mild or acute pain or prescribed on an "as needed" basis.
Pain specialists agree methadone is safe and effective when prescribed by an experienced physician. It also has been safely used to treat heroin addiction in the U.S. since the early 1950s. Millions of addicts have held down jobs and lived for decades while receiving daily doses of the synthetic opiate.

https://www.pewtrusts.org/en/research-and-analysis/blogs/stateline/2015/4/23/most-states-list-deadly-methadone-as-a-preferred-drug
Percentage of prescription opioid overdose deaths involving methadone - United States, 1999-2014:
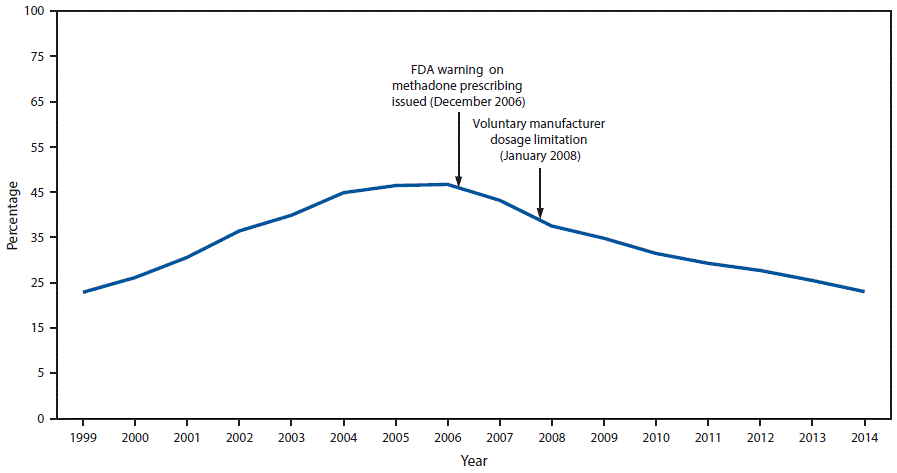

https://www.cdc.gov/mmwr/volumes/66/wr/mm6612a2.htm
Methadone Abuse:
Although methadone is used as a way to curb addiction and reduce cravings, it is an incredibly heavily regulated drug. It is so regulated, that patients who are prescribed methadone in an outpatient setting have to go to a clinic every day to be administered their dose. It is a powerful opiate with potentially addictive qualities. People who start using methadone to overcome their heroin addiction are at a higher risk of abuse because they already have a history of opioid dependency. In fact, for some addicts, methadone is their substance of choice. Methadone does not create the same euphoric effects as heroin or morphine because it is designed to do the opposite; the drug is formulated to block the pleasurable sensations of other opiates. If an individual who is being with Methadone attempts to get high by using heroin, the methadone will, indeed, block the euphoric effects of the heroin (and all other opioids). However, Methadone does have sedative effects, effects which may become euphoric. The euphoric effects are limited; however, they are also great enough that the National Highway Traffic Safety Administration has indicated that Methadone users are "Not fit to drive" due to the side-effects of Methadone.

https://www.addictioncenter.com/opiates/methadone/
Important Information:
You should not use methadone if you have severe asthma or breathing problems, or a blockage in your stomach or intestines.MISUSE OF METHADONE CAN CAUSE ADDICTION, OVERDOSE, OR DEATH, especially in a child or other person using the medicine without a prescription. Keep the medication in a place where others cannot get to it.
Taking opioid medicine during pregnancy may cause life-threatening withdrawal symptoms in the newborn.
Fatal side effects can occur if you use opioid medicine with alcohol, or with other drugs that cause drowsiness or slow your breathing.
Methadone may cause a life-threatening heart rhythm disorder. Call your doctor at once if you have a headache with chest pain and severe dizziness, and fast or pounding heartbeats. Your heart function may need to be checked during treatment.Do not drink alcohol. Dangerous side effects or death could occur.
Avoid driving or operating machinery until you know how this medicine will affect you. Dizziness or severe drowsiness can cause falls, accidents, or severe injuries.Grapefruit may interact with methadone and lead to unwanted side effects. Avoid the use of grapefruit products.
Interactions:
Drug Interactions (649) Alcohol/Food Interactions (2) Disease Interactions (17)
What other drugs will affect Methadone?
You may have breathing problems or withdrawal symptoms if you start or stop taking certain other medicines. Tell your doctor if you also use an antibiotic, antifungal medication, heart or blood pressure medication, seizure medication, or medicine to treat HIV or hepatitis C. Opioid medication can interact with many other drugs and cause dangerous side effects or death. Be sure your doctor knows if you also use:This list is not complete. Other drugs may interact with methadone, including prescription and over-the-counter medicines, vitamins, and herbal products. Not all possible interactions are listed here.
- other narcotic medications - opioid pain medicine or prescription cough medicine
- a sedative like:
- drugs that make you sleepy or slow your breathing - a sleeping pill, muscle relaxer, tranquilizer, antidepressant, or antipsychotic medicine
- drugs that affect serotonin levels in your body - a stimulant, or medicine for depression, Parkinson's disease, migraine headaches, serious infections, or prevention of nausea and vomiting
A total of 649 drugs are known to interact with Methadone.
- 299 major drug interactions
- 340 moderate drug interactions
- 10 minor drug interactions
 Methadone Overview:
Methadone Overview:
https://www.drugs.com/methadone.html
| Side Effects: |
| Get emergency medical help if you have signs of an allergic reaction: hives; difficult breathing; swelling of your face, lips, tongue, or throat. |
|---|
| RxList |
Dolophine (Methadone tablets) Description: https://www.rxlist.com/methadone-hydrochloride-drug.htm |
| Opioid medicine can slow or stop your breathing, and death may occur. A person caring for you should seek emergency medical attention if you have slow breathing with long pauses, blue colored lips, or if you are hard to wake up. |
Call your doctor at once if you have:
|
| Seek medical attention right away if you have symptoms of serotonin syndrome, such as: agitation, hallucinations, fever, sweating, shivering, fast heart rate, muscle stiffness, twitching, loss of coordination, nausea, vomiting, or diarrhea. |
| Serious side effects may be more likely in older adults and those who are malnourished or debilitated. |
| Long-term use of opioid medication may affect fertility (ability to have children) in men or women. It is not known whether opioid effects on fertility are permanent. |
Common side effects may include:
|
| This is not a complete list of side effects and others may occur. Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088. |
Absorption:
Bioavailability: 36-100%. Onset: PO, 0.5-1 hr; parenteral, 10-20 min. Duration: 4-8 hr; repeated administration, 22-48 hr; overdosage, 36-48 hr. Peak plasma time: 1-7.5 hr
Distribution:
Protein bound: 85-90%. Vd: 1-8 L/kg
Metabolism:
Metabolized in liver via N-demethylation
Elimination:
Half-life: 8-59 hr. Excretion: Urine
| Black Box Warnings: |
|---|
Opioid analgesic risk evaluation and mitigation strategy (REMS)
Detoxification and maintenance of dependence
Addiction, abuse, and misuse
Life-threatening respiratory depression
Concomitant use with benzodiazepines or other CNS depressants
Accidental exposure
Neonatal opioid withdrawal syndrome
Life-threatening QT prolongation
Cytochrome CYP450 interactions
Treatment for opioid addiction
|
Overdose:
Because methadone is designed to be a long-acting drug, it can build up very quickly in the body, and that can mean that taking even one more dose than prescribed can lead to an overdose. Unless carefully monitored by a medical professional, methadone use is dangerous, and abuse or addiction can lead to very serious consequences. Methadone's half-life, depending on dose, ranges anywhere from 8 to 59 hours, while the analgesic, or painkilling, effects last up to 8 hours. The long half-life benefits those in recovery from heroin or prescription painkiller addiction, as it stays in the body to ease withdrawal symptoms and cravings. However, this means it is less effective for treating chronic pain conditions related to diseases, such as cancer, multiple sclerosis, or osteoarthritis, because the painkilling effects do not last as long as the drug remains in the body. As a result, individuals who take methadone as a painkiller can put themselves in danger of an overdose if their pain returns before they can safely take their next dose.

https://americanaddictioncenters.org/methadone-addiction
Long Term:
Studies have shown that people who start taking methadone often continue taking it for 20 years or more. The methadone high can create feelings of euphoria and while taking the drug the individual will usually experience pain relief or anywhere from 4-8 hours. Taking methadone actually blocks the things that make people feel high from drugs like heroin and oxycodone. What's important to note with methadone, however, is that with proper dosages, the person taking methadone shouldn't feel a high. Methadone can also have long-term effects on both the brain and the body. The drug can cause intense mood swings and changes in behavior, since the neurotransmitters in the brain are affected by the intake of the drug. Users also may experience depression, confusion, restlessness and agitation. There is also a possibility of a decrease in cognitive function, memory loss and difficulty learning new things. Men and women can also struggle with a reduction in sexual needs and cause sexual dysfunction due to the reduction of testosterone. Severe lung and breathing issues can generate if methadone addiction isn't treated accordingly.

https://www.therecoveryvillage.com/methadone-addiction/
The research is clear: Medication-assisted treatment works
One of the reasons opioid addiction is so powerful is that those in its grips feel like they must keep using the drugs in order to stave off withdrawal. Once a person's body grows used to opioids but doesn't get enough of the drugs to satisfy what it's used to, withdrawal can pop up, causing, among other symptoms, severe nausea and full-body aches. So to avoid suffering through it, people often seek out drugs like heroin and opioid painkillers - not necessarily to get a euphoric high, but to feel normal and avoid withdrawal. (In the heroin world, this is often referred to as "getting straight.")
Medications like methadone and buprenorphine (also known as Suboxone) can stop this cycle. Since they are opioids themselves, they can fulfill a person's cravings and stop withdrawal symptoms. The key is that they do this in a safe medical setting, and when taken as prescribed do not produce the euphoric high that opioids do when they are misused. By doing this, someone significantly reduces the risk of relapse, since he doesn't have to worry about avoiding withdrawal anymore. People can take this for the rest of their lives, or in some cases, doses may be reduced; it varies from patient to patient. The research backs this up

https://www.vox.com/science-and-health/2017/7/20/15937896/medication-assisted-treatment-methadone-buprenorphine-naltrexone
People usually enter methadone treatment because they feel over-whelmed by their dependence on heroin or other opioids:
People dependent on street opioids who receive methadone treatment are healthier and safer than those who do not. They live longer, spend less time in jail and in the hospital, are less often infected with HIV, and commit fewer crimes. Longer periods of methadone maintenance are better than shorter periods. The longer you stay on methadone maintenance, the better the overall outcome. Indefinite treatment often means life-long extension of good health, HIV seronegativity, and freedom from incarceration. Methadone maintenance is treatment for people who are dependent on opioid drugs. It is not a treatment for people whose major problems are with other drugs - such as cocaine, alcohol, benzodiazepines, or cigarettes.


https://www.drugpolicy.org/sites/default/files/aboutmethadone.pdf
Why the methadone doesn't work:
Doling out methadone to heroin addicts has become a daily ritual for many pharmacies but the government needs to tackle the root causes of addiction.

Methadone is a highly addictive synthetic opiate, more addictive than heroin and harder to withdraw from, but it survives the digestive system and so does not need to be injected. Most addicts loathe it. They call it green gunk and grimace as they swallow. All of today's addicts have been coming to the pharmacy for months, some for years. And that's the problem. By the end of the afternoon I have dispensed the gallon of methadone to 33 addicts and supplied three more with clean needles. They should all be back after the weekend.

https://www.theguardian.com/society/2012/jan/10/why-methadone-drugs-dont-work
How do methadone and buprenorphine differ?
Differences between methadone and buprenorphine include the following:
- Methadone is taken as drink, whereas buprenorphine is a pill that is absorbed under the tongue.
- Methadone has a higher risk of overdose than buprenorphine.
- Only those who have completed special training can prescribe methadone, but any physician can prescribe buprenorphine.
- Methadone is most commonly available through specialized treatment clinics; buprenorphine treatment may be easier to access than methadone.
- It can take weeks to reach a fully effective dose with methadone, but only a few days with buprenorphine.
- Side-effects can be more pronounced with methadone.

https://www.camh.ca/en/health-info/mental-illness-and-addiction-index/methadone
The methadone fix:
There is no miracle solution to the addictive grip of opioid drugs such as heroin, writes Patralekha Chatterjee. New WHO guidelines confirm that, even after 40 years, substitution therapies such as methadone are still the most promising method of reducing drug dependence, but getting access to treatment is a global problem. In the global battle against illicit drugs, stemming the crisis of opioid dependence poses a grave challenge.
 Methadone Bulletin of the World Health Organization:
Methadone Bulletin of the World Health Organization:
https://www.who.int/bulletin/volumes/86/3/08-010308/en/
Barriers To Medications For Opioid Addiction:
Opioid use disorder medications are underused for a number of reasons. The medications are inaccessible to many patients because few treatment facilities or health care providers offer them. Stigma, rooted in an erroneous belief that these medications "substitute one addiction for another," often discourages providers from offering, and patients from taking, these medications. Insurance coverage barriers and cost make treatment, including these medications, unaffordable to many patients with Opioid use disorder.

https://www.healthaffairs.org/do/10.1377/hblog20190418.164447/full/
Medicare:
Many older patients rely on surprisingly high doses of opioids for pain relief, which can turn into addiction. One in three older Americans with Medicare drug coverage is prescribed opioid painkillers, but for those who develop a dangerous addiction there is one treatment Medicare won't cover: methadone.
https://www.pbs.org/newshour/health/medicare-doesnt-cover-methadone-treatment-heres-how-congress-may-change-that
Top Definition - Methadone:
A synthetic opiate intended to replace opiate based prescriptions or street drugs, so that an individual can be slowly weaned off and avoid withdrawal symptoms. Often used as a fix between fixes. Its not uncommon for an addict to be on methadone and still using their drug of choice. The doctor put me on methadone because I'm having trouble getting of my meds for my back. I don't have any cash until my pogey comes in, so I'm going to go get my methadone drink.
When You Should Call Your Doctor:
Call immediately if you have chest pain, an irregular or pounding heartbeat, signs of an overdose, withdrawal symptoms, or an allergic reaction. Signs of an overdose are listed on the back of this page. Signs of withdrawal include sweating, runny nose, flu-like symptoms, stomach pain, trouble sleeping, large pupils, irritability, and excessive yawning. Signs of an allergic reaction include a skin rash or hives, trouble breathing, wheezing, chest tightness, and a swollen face or tongue. If you can't reach your doctor right away, seek immediate treatment in an emergency room.


https://www.ismp.org/sites/default/files/attachments/2018-11/Methadonefinal.pdf
Methadone as a Pain Killer: Handle with Care
Few topics in hospital-based pain management generate such diverse viewpoints as the use of methadone as an analgesic. Increasingly ordered by hospice physicians and some hospitalists as a tool for managing difficult pain cases, it is also coming under scrutiny for risks related to cardiac complications, respiratory depression, and the challenges of determining appropriate doses. For some, the risks are grave enough to contraindicate methadone prescription for use in routine hospital practice, unless the hospitalist is well-versed in its use and has access to a pharmacist or other pain expert to review medication orders. Hospitalists should also be aware of the Food and Drug Administration's strongly worded November 2006 Public Health Advisory, "Methadone Use for Pain Control May Result in Death and Life-Threatening Changes in Breathing and Heart Beat."

https://www.the-hospitalist.org/hospitalist/article/123435/methadone-handle-care
Methadone Pain Management Hazard - Respiratory Depression:
The chief serious hazard associated with this opioid when used for pain management is respiratory depression. What makes this particular opioid more problematic than most is that accumulation to steady state can take a week or more. This slow approach to steady state levels brings with it the possibility that side effects can also appear slowly. In the majority of cases, the drug is administered to outpatients; therefore, the patients are unmonitored as the drug accumulates. Specific populations such as the elderly or those prone to abuse of medications may be at particular risk for delayed respiratory depression caused by methadone. Data strongly support the notion that methadone's slow accumulation can have lethal consequences.

https://anesthesiology.pubs.asahq.org/article.aspx?articleid=1933212
Methadone for Diabetic Neuropathic Pain:
It has been our clinical experience that methadone is a unique opioid analgesic that we have found to provide consistently superior analgesia for the treatment of diabetic neuropathy/persistent neuropathic pain, when compared with the other opioids currently available, without sacrificing safety or tolerability.

https://care.diabetesjournals.org/content/28/2/485
Other Medical Problems:
Make sure you tell your doctor if you have any other medical problems, especially:
- Alcohol abuse, or history of
- Brain tumor
- Breathing or lung problems (eg, COPD, cor pulmonale, hypercapnia, hypoxia, apnea, sleep apnea)
- Depression, history of
- Drug dependence, especially narcotic abuse or dependence, history of
- Gallbladder disease
- Head injuries, history of
- Heart disease (eg, cardiac hypertrophy)
- Heart rhythm problems (eg, arrhythmia, long QT syndrome), or history of
- Hypokalemia (low potassium in the blood)
- Hypomagnesemia (low magnesium in the blood)
- Increased pressure in your head
- Stomach or bowel problems
- Weakened physical condition - Use with caution. May increase risk for more serious side effects
- Hypotension (low blood pressure)
- Pancreatitis (inflammation of the pancreas)
- Seizures, history of - Use with caution. May make these conditions worse
- Kidney disease
- Liver disease - Use with caution. The effects may be increased because of slower removal of the medicine from the body
 Methadone (Injection Route):
Methadone (Injection Route):
https://www.mayoclinic.org/drugs-supplements/methadone-injection-route/description/drg-20475103
Prescribed for:
What Conditions does it Treat?
- Symptoms from stopping treatment with opioid drugs
- Dependence on opioid-type drugs
- Severe chronic pain requiring long-term opioid treatment
Uses:
This medication is used to treat severe ongoing pain (such as due to cancer). Methadone belongs to a class of drugs known as opioid analgesics. It works in the brain to change how your body feels and responds to pain.Do not use this medication to relieve pain that is mild or that will go away in a few days (such as pain from surgery). This medication is not for occasional ("as needed") use.
This medication is also used to treat addiction to opioids (such as heroin) as part of an approved treatment program. It helps prevent withdrawal symptoms caused by stopping other opioids.Before using:
Tell your doctor or pharmacist your medical history, especially of:
- Brain disorders (such as head injury, tumor, seizures)
- Breathing problems (such as asthma, sleep apnea, chronic obstructive pulmonary disease-COPD)
- Kidney disease
- Liver disease
- Mental/mood disorders (such as confusion, depression, thoughts of suicide)
- Personal or family history of a substance use disorder (such as overuse of or addiction to drugs/alcohol)
- Stomach/intestinal problems (such as blockage, constipation, diarrhea due to infection, paralytic ileus)
- Difficulty urinating (such as due to enlarged prostate)
- Disease of the pancreas (pancreatitis)
- Gallbladder disease
Precautions:
- This drug may make you dizzy or drowsy
- Alcohol or marijuana (cannabis) can make you more dizzy or drowsy
- Do not drive, use machinery, or do anything that needs alertness until you can do it safely
- Avoid alcoholic beverages.
- Talk to your doctor if you are using marijuana (cannabis).
Methadone may cause a condition that affects the heart rhythm (QT prolongation). QT prolongation can rarely cause serious (rarely fatal) fast/irregular heartbeat and other symptoms (such as severe dizziness, fainting) that need medical attention right away.
Some products may contain sugar. Caution is advised if you have diabetes.
WARNINGS:
Methadone has a risk for abuse and addiction, which can lead to overdose and death.
Methadone may also cause severe, possibly fatal, breathing problems and heartbeat problems.
To lower your risk, your doctor should have you take the smallest dose of methadone that works, and take it for the shortest possible time. Do not increase your dose or take this medication more often than directed.The risk for severe breathing problems or heartbeat problems is higher when you start this medication, when you are switching from another opioid to methadone, after a dose increase, or if you take the wrong dose/strength.
Breathing problems from methadone may not happen right away after taking a dose. Most heartbeat problems have happened in people using large doses of methadone for pain relief, but this problem can also occur in people taking smaller doses to treat opioid addiction.Taking this medication with alcohol or other drugs that can cause drowsiness or breathing problems may cause very serious side effects, including death.
Also, other medications can affect the removal of methadone from your body, which may affect how methadone works. Be sure you know how to take methadone and what other drugs you should avoid taking with it.Get medical help right away if any of these very serious side effects occur: slow/shallow breathing, unusual lightheadedness, severe drowsiness/dizziness, difficulty waking up, fast/irregular heartbeat, fainting.
User Reviews:
1138 Total User Reviews Methadone Oral:
Read ReviewsCondition: Pain (648 Reviews): Effectiveness (4.10) Ease of Use (4.38) Satisfaction (3.95)
 Methadone HCL (Methadose):
Methadone HCL (Methadose):
https://www.webmd.com/drugs/2/drug-2671-1278/methadone-oral/methadone-concentrate-oral/details
| Maximum Dosage: | |
|---|---|
| Prescribers Digital Reference | |

Dolophine - Drug Summary: https://www.pdr.net/drug-summary/Dolophine-methadone-hydrochloride-727 | |
| With appropriate dosage titration, there is no maximum dose of methadone. Safety and efficacy in pediatric patients have not been established; however, methadone is used off-label in these populations. |
Street Names: Fizzies, Amidone, Chocolate Chip Cookies


https://www.accessdata.fda.gov/drugsatfda_docs/label/2016/006134s040s041lbl.pdf

https://www.ncbi.nlm.nih.gov/books/NBK548084/

https://www.ncbi.nlm.nih.gov/books/NBK501233/
https://www.samhsa.gov/medication-assisted-treatment/treatment/methadone
Taxis, methadone patients, millions of tax dollars at center of Medi-Cal fraud investigation - At least two public agencies in Silicon Valley are investigating alleged fraud involving California’s Medi-Cal program. At issue are millions of tax dollars that have spent transporting patients to a ... Wednesday May 06, 2026 - msn.com ‘Golden handcuffs’: Wisconsin methadone rules limit access to opioid treatment - After years of opioid use, Bob saw three paths ahead: jail, death or methadone. The 70-year-old Stevens Point resident chose methadone, which he has stuck with for more than half his life. He credits ...
| ||
| Opioids | Link to this page |