[ Home ] [ Controlled Substances ] [ Hallucinogens ]
IBOGAINE
|
Ibogaine History:
Ibogaine was first discovered in Africa, though not as it is synthesized today. The Pygmy tribe, native to West Africa, would often use the drug in its purest form during religious ceremonies. The drug comes from a tree known as the iboga tree, from which the drug also gets its name. The tribe would pull the roots and bark from the tree, and chew on them in order to achieve a psychedelic state. The drug was often used to enhance religious ceremonies and rituals performed by the tribes. Ibogaine was reportedly so powerful that users lost control of their bodily functions, and needed buckets or diapers nearby in the event that the trip was too intense. When western researchers visited the tribes, they noticed the psychedelic effects that the drug was having on the Shamans and wondered what else, if mixed with other compounds, the drug was capable of. They had almost no idea what they were getting into but brought the drug home for synthesis anyway.
In the 1930s, before ibogaine was officially synthesized, the French began to market it as a stimulant under the name Lambarene. The drug quickly became popular among athletes, as it resulted in increased energy and lack of fatigue. However, doctors soon realized there was the potential for cardiovascular injury with long-term use, so Lambarene was quickly pulled from the market. Researchers were no longer allowed to sell and market the drug, but behind the closed doors of their labs, they continued to test and synthesize the drug. By the mid-60s, they had found a viable, stable form of ibogaine.
Around the same time, a 19-year-old heroin addict accidentally realized that there may be more to ibogaine than researchers realized. The teenager, Howard Lotsof, had taken the drug recreationally with four of his friends after hearing of its psychedelic properties. Coincidentally, as he was getting high on ibogaine, he noticed that his cravings for heroin had subsided. His friends echoed his feelings and additionally noted that they weren't feeling withdrawal symptoms either. Before long, the young enterprising addict had come up with a patent for ibogaine and had signed a contract with a Belgian company to produce ibogaine in tablet form with the intent of treating addiction. Clinical trials took off in the late 80s and showed promise in reducing withdrawal symptoms in addicts. But when a 24-year-old woman was given too high a dosage in 1993 and died, the trials were shut down.
Though it's no longer used to treat addiction (despite many experts pushing for it), rumors abound that throughout history it has been used in other sectors - most notably the MKUltra experiments.
In the early 50s and 60s, the Central Intelligence Agency conducted a series of experiments known as MKULTRA, that pushed the boundaries of the human mind, not to mention medical ethics. One section of the experiments revolved around the prospect of mind control, and the possibility that it could be done with drugs. According to some, ibogaine was one drug used for MKULTRA. Due to the drug's tendency to make one more attune with others' feelings, many believed that it could be adapted for mind control. When under the influence of ibogaine, one goes through a three-stage high. In the first, known as the "acute" phase, the user becomes hyper aware of their surroundings. A "panoramic" view of past memories has been reported, along with reports of meetings with a transcendent being. During this phase, the user is easily influenced.
During the second and third phases, which can last between 12 hours and three days, the user's high starts to wear off, but their hyper-awareness of their surroundings and their heightened willingness to discuss their introspection remain. The user's pliability during these stages further increases the drugs likelihood as a mind-control substance. Of course, as most of the MKULTRA documents were destroyed, redacted, or can't be found, there's no way to tell how large a part, if any, ibogaine played.
Today, researchers in the field of psychedelics are still pushing for ibogaine to be used as an opioid-dependency cure, though movements are so far, slow.
https://allthatsinteresting.com/ibogaine
Ibogaine is a psychoactive drug that induces hallucinogenic effects like those associated with use of LSD or psilocybin. While the drug can lead to some short-term side effects, including anxiety after experiencing hallucinations, it has been touted for a few years as a potential solution to devastating addiction problems. Anecdotal evidence suggests that ibogaine, which is derived from a plant found in the African rainforest, adjusts brain chemistry to the point that a person who otherwise might experience intense withdrawal symptoms for one or two weeks does not go through withdrawal or suffer from cravings.
However, scientists exploring the potential of this drug in addiction treatment do not believe ibogaine completely ends addiction; instead, it interrupts the process.

https://americanaddictioncenters.org/meth-treatment/success-rate-for-ibogaine
In lower doses, ibogaine acts as a stimulant, increasing energy and decreasing fatigue in a way that is distinct from other central nervous system stimulants like amphetamines and cocaine.2 In larger doses, ibogaine produces oneirogenic effects, meaning that it stimulates a dream-like state while awake, as well as closed eye imagery and the retrieval of repressed memories. The occidental use of ibogaine, especially its application in the treatment of substance use disorders, was pioneered by Howard Lotsof. In 1962, 19 year old Lotsof serendipitously found that a single dose of ibogaine not only interrupted his physiological dependence on heroin, it also took away his craving to use, all with no withdrawal symptoms. Lotsof spent the rest of his life advocating for the development of ibogaine as a prescription medicine.
Ibogaine has been used therapeutically for several indications, particularly detoxification from opiates. It has been shown to decrease the self-administration of stimulants, opiates and alcohol, as well as to significantly reduce the withdrawal symptoms from opiates after a single administration. Other research shows a reduction of developed tolerance to opiates and alcohol, and a significant decrease in cravings for opiates and cocaine for an extended period of time after treatment.

https://www.ibogainealliance.org/ibogaine/
Lotsoff's drug seemed to be working as two-thirds of 30 patients worldwide remained abstinent from drugs for several months and even years in contrast to the general 75 percent relapse rate within six months with traditional methods. Initially, NIDA was interested in ibogaine, and the U.S. Food and Drug Administration (FDA) approved clinical trials for using the drug in opioid dependency treatment; however, a lack of funds and the death of a patient using ibogaine in the Netherlands effectively halted research in the mid-1990s and ibogaine remains a banned substance in America today. Around the time the United States declined to further ibogaine research, private clinical trials and ibogaine treatment clinics sprang up in other parts of the world.
Researchers today are attempting to isolate noribogaine, one of the metabolites of ibogaine, and hoping to test its effectiveness as a potential legal alternative to ibogaine for addiction treatment.

https://www.therecoveryvillage.com/opiate-addiction/treatment-rehab/using-ibogaine
In 1981, 44 kg of iboga extract was produced by an unnamed European manufacturer. The entire stock was purchased by a single buyer, Carl Waltenburg, who distributed it as "Indra extract" to treat heroin addicts in Christiania, Denmark, a small village with a high number of heroin addicts. A number of local movements took hold in the early- to mid-1990s in offshore locations from the US, mostly aimed at treating heroin addicts. In total, more than 3,000 private clinics and retreats were established and an entire "medical subculture" flourished. Numerous accounts of individuals fighting and overcoming addiction surfaced.
Today, while ibogaine is illegal in the United States, primarily due to the regulatory difficulty in reclassifying a Schedule I drug, it is available as a prescribed anti-addiction treatment in many countries, including Canada, South Africa, the Netherlands, Mexico, Norway, and the U.K. among others.
Effects of larger doses
One of the most immediate adverse effects you may feel is ataxia, or an inability to fluidly coordinate muscle movements. Nausea, dry mouth, dizziness, and vomiting can also occur. It's best to lay down while tripping on ibogaine as sudden movements can lead to increases dizziness and nausea. You can expect to be in bed for the first 12 hours of your trip. The first several hours will be intense before you start to come down as your body metabolizes the ibogaine.
A trip can be broken down into three phases:
- Acute, "awakened dream state" phase. Begins 1 to 3 hours after taking ibogaine and can last 4 to 8 hours. Most report a "panoramic," mostly visual experience of past memories.
- Evaluative or reflective phase. Begins approximately 4 to 8 hours after taking ibogaine and can can last 8 to 20 hours. Attention is directed at evaluating the experiences of the acute phase. Many prefer as little environmental stimuli during this phase and the acute phase as it's easy to become agitated or annoyed by distractions.
- Residual stimulation phase. Begins approximately 12 to 24 hours after taking ibogaine and can last 24 to 72 hours or more. Attention shifts back to the external environment during this phase while the subjective psychoactive experience begins to fade. Normal movement returns and people often report heightened arousal and vigilance during this period as well. Some report a reduced need for sleep for several days to weeks following treatment.

https://thethirdwave.co/psychedelics/ibogaine/
Ibogaine is a psychedelic chemical found in the West African shrub Iboga. Bizarre in chemical structure and psychoactive properties, the drug remains mysterious to scientists and psychonauts alike. At high doses, ibogaine causes intense, unforgivingly introspective and dream-like hallucinatory experiences that can last upwards of 24 hours. The African psychedelic might have remained nothing more than a curiosity in the West if not for the discovery of its ability to disrupt physical and psychological drug addiction. Thousands of anecdotal reports and preliminary scientific research provide evidence that a single dose of ibogaine can eliminate both withdrawal symptoms and craving in drug addicts1. In the United States, ibogaine remains a schedule 1 drug, and those seeking treatment must pilgrimage to countries that do not regulate it or take a chance with illegal underground treatment centers. What will it take for ibogaine to become medically available in the United States?

https://psychedelicstoday.com/2019/04/22/future-medical-ibogaine/
Ibogaine acts as a mild stimulant in small doses. In large doses, it can put a person into a severe psychedelic state. Some people have found that large doses reduce opiate withdrawal symptoms and help with substance-related cravings. People with substance use addictions have found that large doses of it can reduce withdrawal from opiates and help rid them of their substance-related cravings. In many cases, however, the effects are short-lived. The safety of this treatment is also in question. Most studies have been in animals. In humans, there have been serious side effects, including unexplained deaths that may be linked to the treatment.

https://www.healthline.com/health/ibogaine-treatment
A large dose of ibogaine can prevent opioid withdrawal, eliminating cravings for drugs like prescription painkillers and heroin for up to months at a time - making it a potent tool for detox. And the psychedelic experience can cause what users describe as a profound shift in perspective, allowing them to see their life more clearly and make important adjustments for the better. Ibogaine doesn't cure addiction, but it can help addicts put themselves in the right mindset and setting. There are limits to ibogaine, of course. For one, it doesn't cure opioid addiction. But the detox effect, coupled with the perspective attributed to the psychedelic trip, allowed patients to get their lives back in order - and more easily avoid drugs.
"The hallucination is really important," Steve said. "It lets you unplug, where there's no cellphones, no anxiety, money has no meaning, all possessions in your life have zero meaning. So you're sitting in a dark room, and you can sit there and talk to your inner self and figure out what's truly important in your life."
Ibogaine's detox effects and hallucinogenic experience make it easier for addicts to find that good environment: With fresh perspective and no cravings calling them back to heroin, addicts stand a much better chance of recovery. This gets to one of the nuances of drug abuse: Addicts can't, in many situations, just quit drugs. They also often need to change the mentality and environment in which they were hooked - or risk falling into old, bad habits again.

https://www.vox.com/2015/9/14/9314315/ibogaine-treatment
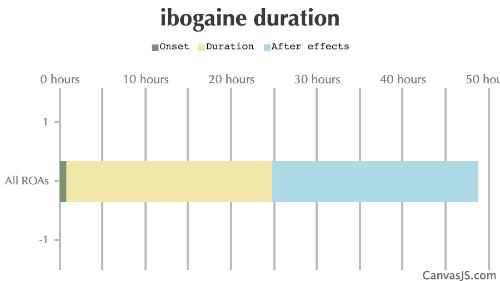
| Duration: An alkaloid found in many African plants most famously Iboga, with psychedelic and hallucinogenic properties. May be unpleasant. Traditionally used in tribal environments for coming-of-age rituals, it has recently been used as an alternative treatment for drug addiction although this usage has not been backed by conclusive data in humans. Has killed in overdose. | |||
| Route | Onset | Duration | After Effects |
|---|---|---|---|
| Tripsit Factsheets | |||

Ibogaine Basic Information: http://drugs.tripsit.me/ibogaine | |||
| All ROAs: | 45-180 minutes | 24-30 hours | 24-72 hours |
| |||
| Aliases: iboga | |||
| Effects: Euphoria, empathy, insight, brightened colour, Closed/Open eye visuals, enhanced tactile sensation, mental/physical stimulation, decreased appetite, pupil constriction, restlessness, change in perception, ego softening, sweating/chills, muscle tension, confusion, insomnia. | |||

https://www.psychologytoday.com/us/blog/ending-addiction-good/201410/the-potential-ibogaine-in-treating-substance-abuse?quicktabs_5=0

https://www.psymposia.com/magazine/is-ibogaine-the-cure-for-opioid-addiction-its-not-that-simple/
MAPS has completed two observational studies of the long-term effects of ibogaine treatment on patients undergoing therapy at independent ibogaine treatment centers in Mexico and New Zealand.
https://maps.org/research/ibogaine-therapy

http://www.maps.org/news-letters/v13n2/v13n2_16-21.pdf

http://www.maps.org/news-letters/v15n1/iboga21.pdf
Some proponents of ibogaine blame its unavailability in the U.S. on the pharmaceutical industry for not developing and marketing the drug. They argue that Big Pharma has the funding necessary to vet ibogaine to the FDA's satisfaction, but drug companies choose not to do so because it wouldn't make good business sense. Research trials like Mash's are often financed by pharmaceutical companies. Beyond this issue of research funding, lobbying efforts for the reclassification of ibogaine would be more effective coming from pharmaceutical companies than from the recovery community. Congress is not known for its keen responsiveness to the pleas of heroin addicts. Big Pharma's development of ibogaine might be a great thing. Why blame the companies, though, for not pursuing something they don't deem in their best interests? Unregulated ibogaine treatment is not without danger, but neither is being a heroin addict.

https://abovethelaw.com/2014/02/whos-to-blame-for-ibogaine-a-debate-over-whether-big-government-or-big-pharma-is-keeping-heroin-addicts-from-getting-well/
The theory is that ibogaine works by filling in opiate receptor sites, which ends cravings for the drug and effectively hits the reset button on the brain's neurotransmitter mechanisms. At the same time, the liver metabolises it into noribogaine, which is thought to have powerful detoxifying and anti-depressant properties. This further helps eliminate the pain and danger associated with withdrawal. In the US, ibogaine is designated under Schedule 1 due to its "high potential for abuse or addiction and no known medicinal applications", but this is patently ridiculous. Unlike other treatment substances such as methadone, ibogaine is in fact nonaddictive and doesn't need to be taken on a continuing basis. Its effectiveness makes its medicinal value obvious, and it has virtually no abuse potential - it is incredibly expensive and comes with some unfortunate short-term side-effects such as heavy nausea. Even Timothy Leary said, "It'll never be a party drug."
Unfortunately, however, ibogaine is an extremely powerful hallucinogen with some alarming and potent side-effects including neurotoxicity (body tremors, postural instability and ataxia), cardiac effects (reduced heart rate and blood pressure, and interruptions to the heart's electrical system), cardiotoxicity, nausea and vomiting. Studies have suggested there is a significant risk of brain damage associated with high dosages, and there have been at least 12 documented deaths linked to its ingestion.
Ibogaine is not an approved drug in New Zealand. Ibogaine's day may come, but until we know more about it and how to use it safely, we are better off sticking with proven treatments.

https://www.drugfoundation.org.nz/matters-of-substance/may-2011/should-ibogaine-be-an-approved-drug-treatment/

https://www.drugwarfacts.org/chapter/ibogaine
https://www.webmd.com/vitamins/ai/ingredientmono-440/iboga

https://www.drugs.com/npp/iboga.html
https://www.rxlist.com/iboga/supplements.htm
If you are interested in partaking in an iboga session for addiction treatment, psychotherapy or personal growth, there are very important issues of which you should be aware. This ethnobotanical can have a vast therapeutic potential if used in controlled conditions, as well as some important risks if used unprofessionally. Here you find information about important issues involved in the use of iboga.

https://www.iceers.org/interested-in-taking-ibogaine/

https://erowid.org/experiences/subs/exp_Ibogaine.shtml

https://drugs-forum.com/tags/ibogaine/

https://www.reddit.com/r/Ibogaine/
There is a lot of bad information online about Ibogaine. It's truly not a fun experience - quite the opposite. It's also very dangerous if done improperly. That said, it will reset your receptors!

https://twitter.com/hashtag/ibogaine?lang=en


http://the-eye.eu/public/Psychedelics/Psychedelic%20Praxis%20Library%203.0/Collections%20by%20Substance/Ibogaine/1996%20-%20Rienzo%20-%20The%20Ibogaine%20Story-%20Report%20on%20the%20Staten%20Island%20Project.pdf
Ibogaine:
Ibogaine is a naturally occurring psychoactive substance found in plants in the family Apocynaceae such as Tabernanthe iboga, Voacanga africana, and Tabernaemontana undulata.
- A psychedelic with dissociative properties
- Used as an alternative medicine treatment for drug addiction in some countries
- Also used to facilitate psychological introspection and spiritual exploration.
- Although it was first commonly advertised as having anti-addictive properties in 1962, its Western use predates that by at least a century.
- In France, it was marketed as Lambarene and used as a stimulant.
- The total synthesis of ibogaine was described in 1956.
Preliminary research indicates that it may help counter drug addiction.
The psychoactivity of the root barks of the iboga tree (Tabernanthe iboga), from which ibogaine is extracted, was first discovered by the Pygmy tribes of Central Africa, who passed the knowledge to the Bwiti tribe of Gabon. French explorers in turn learned of it from the Bwiti tribe and brought iboga back to Europe in 1899-1900, where it was subsequently marketed in France as Lambarene.
the U.S. Central Intelligence Agency (CIA) studied the effects of ibogaine in the 1950s
Its use has been associated with serious side effects and death. Between the years 1990 and 2008, a total of 19 fatalities temporally associated with the ingestion of ibogaine were reported, from which six subjects died of acute heart failure or cardiopulmonary arrest.
Ibogaine is a banned hallucinogenic drug. Scientists believe it can help veterans overcome PTSD - Trials on veterans suggest the potent hallucinogen could provide a new treatment for PTSD, but scientists still don't know how it works. Thursday May 14, 2026 - bbc.com Trump eased restrictions on research for ibogaine. Here's what to know about the psychedelic drug. - The drug is gaining favor in scientific circles for its ability to curb some substance-abuse disorders. Oklahoma Lawmakers Pass Ibogaine Bill, Sending Psychedelic Reform To Governor’s Desk - This bill is more than a policy change—it offers real hope to so many people who desperately need it.” By Jack Gorsline, Filter The Oklahoma State Senate voted on April 29 to pass the Oklahoma ... Ibogaine for Alzheimer’s Disease? Why Brain Experts Are Paying Attention - If you've watched a loved one struggle with Alzheimer's disease or memory loss, you know how heartbreaking it can be—and how desperately we need new solutions. An ancient plant-based remedy called ... Veteran: Executive Order a Win for Ibogaine, But More Research Needed - A former Navy SEAL who used psychedelic drugs to overcome severe PTSD hopes new opportunities for research and treatment can help other veterans. Joe Rogan exaggerates efficacy of psychedelic ibogaine for treating opioid addiction - Studies show that ibogaine can be effective for short-term opioid addiction treatment, especially reducing drug cravings and some withdrawal symptoms. Trump signs order to speed review of psychedelics, including the controversial drug ibogaine - Ibogaine and other psychedelics remain banned under the federal government’s most restrictive category for illegal, high-risk drugs. Ibogaine is drawing new interest from the Trump administration. Here’s what to know about the psychedelic - Psychedelic drugs, once pushed to the fringes of medicine, are gaining serious attention within the Trump administration as potential treatment options for people with certain mental health conditions ...
| ||
| Hallucinogens | Link to this page |